Currently, mammograms are the standard for breast cancer detection in women. Women over 50 are recommended to undergo mammographic detection on a regular basis, usually about once a year.
These tests take an X-ray of the breast and have primarily been criticized for the false positives they can produce. These false positives waste money and resources, forcing the patients to undergo unnecessary biopsies – a source of great personal stress for the patient.
Doctors continually recommend mammograms (perhaps most recently Vancouver radiologist Dr. Ian Gardiner, according to the Vancouver Courier) but for the average female, one size does not fit all. And, as the CBC recently posted, mammograms save one life for every three unnecessary treatments.
With a constant stream of new reports about how mammograms save lives, it can be confusing for the average woman to navigate the radiological landscape. Sometimes we get to choose which method of imaging we want for ourselves, but for the most part, in Canada, we get lumped in with the masses and sent to get a mammography.
A more concerning issue, however, is that mammograms can also produce false negatives. It is obviously more dangerous to have cancer without knowing it than to diagnose something that is not there. Missed detection leads to the continual growth of cancer, making it more difficult to cure in the future if and when that cancer is eventually detected.
While a major factor in mammogram false positives is breast density, dense breasts can equally cause false negatives in mammogram tests, increasing the risk of breast cancer. The fact that this is not widely known is alarming.
Are You Dense? is an American group and movement that focuses on illuminating these issues. Their website is filled with survival stories from a group of women determined to inform the public and to work to pass bills. According to Are You Dense?, dense breasts are composed of tissue that has less fat and, therefore, show up white on a mammogram so the tumours are hardly visible on an X-ray.
Their website states that dense breasts occur in 40 per cent of women over the age of 40 and that tumours are 40 per cent undetectable with a mammogram for women with dense breasts. However, doctors continue to use these mammograms on women who may have dense breasts. A mammogram or an MRI (magnetic resonance imaging) can test for dense breasts, but doctors are not required to tell their patients about this issue.
In the U.S., fives state have passed the Simitian Breast Cancer Detection Bill, indicating that doctors must tell their patients about the pitfalls of dense breasts, screen for dense breasts, and inform patients if they have dense breasts. Virginia, New York, Connecticut, Texas, and California have all passed this bill, with many other states appearing to soon follow suit. This also allows the patients to turn to other methods to detect tumours.
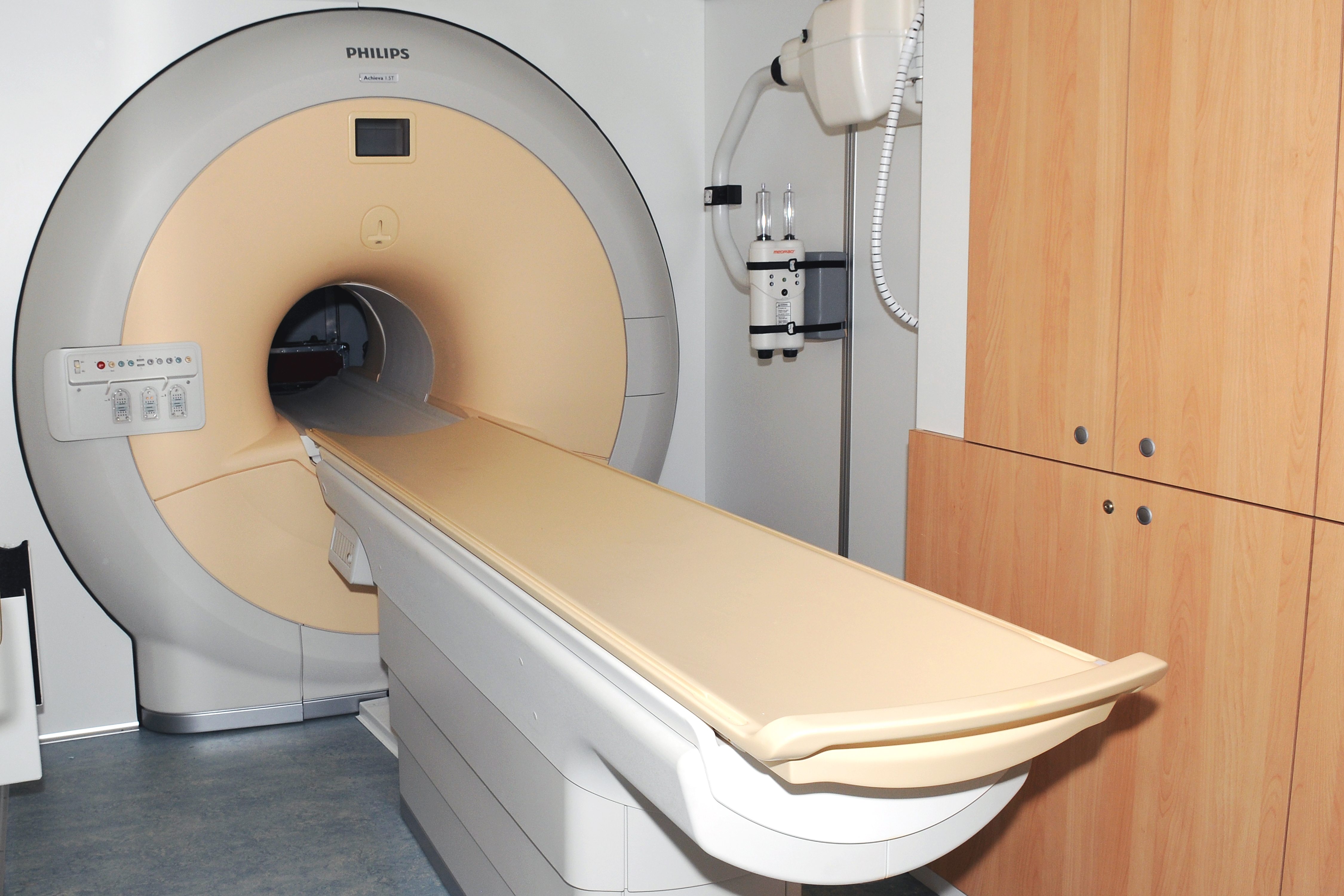
Ultrasounds, which use a transducer on gel-covered skin to image a particular organ, can be used to add value to the mammograms, and they do not expose patients to radiation. Magnetic resonance imaging, which is a large magnetic imaging station, is an obvious alternative because it is more accurate in assessing dense breasts. Since it is much more expensive, though, it has not yet been adopted as the go-to method of breast cancer detection.
Thermography, according to CBC news, is also an option but has caused major problems of both false positive and negative results, and has been deemed by many as useless. It takes images using a camera sensitive to heat.
The United States still widely uses mammograms, but has also moved to MRIs and breast specific gamma imaging, which uses a gamma camera to take pictures. Both of these do not give exposure to radiation. The Canadian health care system has adopted a practice that does not benefit every patient equally, as those with dense breasts or implants have a disadvantage that is unknown to them.
Although mammograms do save lives and acquire accurate results for women without dense breasts, there needs to be another go-to mode of detection for women with dense breasts that does not blind its patients into thinking they are cancer-free each time they get a negative diagnosis. Mammograms do not need to disappear completely: they do have a purpose as long as they save lives.
Canadians, however, need to demand more expensive equipment because it will save lives in the long run. With the occurrence of false negatives, more extensive cancer treatment is used since the cancer is then found later and will have progressed. Canada needs to make better decisions in the detection of breast cancer and put more money into detection so that less money is necessary in the treatment itself.
We can’t just rely on our health care system to provide the most valuable care; we need to demand it ourselves. So, women: don’t just accept a negative mammogram diagnosis, demand more options, such as MRI and gamma imaging.